Access to all articles, new health classes, discounts in our store, and more!
Isolation From Milk Supplies of Specific Types of Green-Producing (Alpha) Streptococci and Their Thermal Death Point in Milk
Read before the meeting of the Southern Minnesota Medical Association, August 23, 1943. Published in Minnesota Medicine, Vol. 27, No. 6, pp 469-474 and No. 7, pp 550-556. June-July, 1944.
* * *
During studies on the etiology of various diseases,8,10,12,13,14,17,27 it was found that culture mediums in common use often did not suffice for the isolation of causative strains of alpha streptococci or for the maintenance of their specific properties. Mediums which I have found especially favorable for the primary isolation and maintenance of characteristic properties of pathogenic alpha streptococci were dextrose-brain broth and soft dextrose-brain agar.
The etiologic relation of streptococci and other organisms found in raw milk to various diseases is well recognized. There is a growing conviction among health officers and physicians, especially pediatricians, that pasteurization of milk by present-day methods does not always suffice to prevent epidemic infection.32 Ayers and Johnson3 consider pasteurization, as now practised, to be a method of obtaining the thermal death point of only a majority of organisms.
It occurred to me that the mediums found highly favorable for the isolation of causative alpha streptococci from persons ill might also be more suitable than ordinary mediums (1) for the isolation of pathogenic streptococci from milk supplies and (2) as test mediums to determine the thermal death point in milk of alpha streptococci. Accordingly, comparative cultures were made in dextrose-brain broth, dextrose broth and on blood-agar, from samplings of raw and pasteurized milk supplies, from raw milk after pasteurization under controlled conditions in the laboratory, from commercially pasteurized milk after repasteurization, from samplings obtained in a sterile manner directly from cows, and from suspensions of streptococci that had been heated in milk to 63, 68 and 73° C., respectively, for thirty minutes.
It is my purpose at this time to describe the methods used and to report the results obtained in an extended study on the virulence, cataphoretic velocity, serologic properties and heat-resistance of green-producing or alpha streptococci isolated from milk supplies during epidemics and remote from epidemics, and to indicate a pasteurizing temperature which invariably kills specifically virulent alpha streptococci commonly found in milk supplies.
Methods
Samples of milk from supplies studied were obtained through the cooperation of physicians, health officers, hospital superintendents and dairymen and represented a very wide range of conditions as to size and type of epidemics, season, climate, size of dairies and different methods of pasteurization and refrigeration. These included samplings from supplies during studies of eight major epidemics of poliomyelitis, four major epidemics of encephalitis, five distinct outbreaks of persistent epidemic hiccup and seven major epidemics of influenza, in addition to supplies studied during minor outbreaks and in many individual cases. Most of the samples were from grade A supplies and the bacterial content was checked by the constituted authorities and myself by present-day standard methods. The milk had been pasteurized by the holding and flash methods. Inspection of herds for evidence of disease of the udder and in regard to cleanliness in the handling of the milk likewise had been made in the usual manner. Results that were considered as having epidemiologic importance were reported immediately to the constituted authorities in question.
Cultures were made chiefly in tall tubes of dextrose-brain broth, soft dextrose-brain agar, dextrose broth and autoclaved litmus milk, each containing 20 c.c. of medium, and on blood-agar plates. The dextrose-brain broth and soft dextrose-brain agar (0.2 per cent agar) were prepared from 0.2 per cent dextrose broth to which Andrade’s indicator (1 c.c. of indicator to 1,000 c.c. of broth) had been added. Pieces of fresh calf brain (approximately 1 part of brain substance to 6 parts of medium) were added to tall columns (10 to 12 cm.) of the medium in tubes or bottles. The reaction of the dextrose broth was brought to pH 7.2 and after the brain substance had been added, the mediums were autoclaved at 20 pounds’ pressure for twenty minutes.
Dextrose-brain broth, dextrose broth and autoclaved litmus milk were inoculated routinely with 2 c.c. of the different samples of milk under study and 0.05 c.c. of the milk was spread on blood-agar plates. After it was found that epidemic strains of streptococci isolated from patients grew in much higher dilution than nonepidemic strains, when subjected to the serial dilution method16 in the brain-containing mediums, this method was also used in culturing milk to compare colony counts obtained in this way with cultures on blood-agar and with counts obtained by the standard milk-agar plate method.1
The serial dilution method,16 in which it was found that virulent streptococci often grew in far higher dilution than did saprophytic organisms, was also used to obtain pure cultures of streptococci especially suitable for inoculation into animals and for serologic studies. By this method, cultures were made routinely alternately in dextrose-brain broth and dextrose-brain agar, beginning with dextrose-brain broth, thus using four tubes of dextrose-brain broth and three tubes of dextrose-brain agar, or in successive tubes of dextrose-brain agar, each tube containing about 20 c.c. of medium. Just before inoculation, the tubes of mediums were steamed for fifteen minutes in the autoclave and then cooled to 40° C. The first tube in the series was inoculated either with 2 c.c. of milk from a 3 c.c. pipet, making a dilution of 1:10 (10-1), or with a 26-gauge nichrome wire 14 cm. in length; which was dipped into the milk or culture for a distance of 12 cm. and to which there adhered approximately 2 c.mm. of liquid, making a dilution of 1:10,000 (10-4). Two-tenths cubic centimeter, by the pipet method, or 2 c.mm., by the wire method, was transferred serially to the remaining six tubes, at intervals of ten to twelve seconds, making dilution increments of 10-2 or 10-4, respectively, at every step. Thorough mixing of the inoculum in each tube was accomplished by rapidly filling and emptying the pipet six times with a rubber bulb of 3 c.c. capacity and by twirling the wire vigorously in each tube. The same pipet was used throughout each series of dilutions and the wire was sterilized in the Bunsen flame only before and after the first transfer. It is to be understood that dilutions made in this way represent dilution of liquids and not necessarily of organisms.
The serial dilution cultures were made in a nonstacked bacteriologic hood under conditions in which control cultures made of sterile material never yielded streptococci. All inoculated mediums were incubated at 34° C. (93.2° F.). Cultures were examined daily for evidence of growth and films were made, stained by Gram’s method and counterstained with 2 per cent aqueous solution of safranine 0, and examined microscopically for type of organisms.
Cultures showing streptococci in dextrose-brain broth and dextrose-brain agar were plated routinely on blood-agar to determine their type. The solubility in bile or sodium taurocholate of saline suspensions of the streptococci isolated was tested by the usual methods. The fermentative power of the streptococci isolated was not studied routinely because preliminary studies did not show any correlation between fermentative power and specific virulence, serologic reactions or distribution curves of cataphoretic velocity.
Studies on the resistance of streptococci to heat were made by heating 5 or 10 c.c. of milk naturally contaminated with streptococci and by adding the streptococci to 5 or 10 c.c. of autoclaved milk in glass ampules or bottles. After inoculation the ampules were sealed in the Bunsen flame and the bottles were sealed with sterile, overhanging rubber stoppers. Both were submerged in a water bath during the heating period. Certified thermometers were used to check the temperature in different parts of the pasteurizing bath and of milk contained inside of two ampules or bottles throughout the heating period. In order to be sure that the temperature was the same for each sampling, the water bath containing the samples or bottles was shaken on a shaking machine during the heating period. The temperature of the water in the bath and of the milk in ampules or bottles was increased slowly, so that approximately fifteen minutes were required to bring the temperature from about 25° C. (77° F.) to the required point, or the ampules or sealed bottles were added to the previously heated water, thus simulating the principles used in the commercial holding and flash methods of pasteurization. The heating period of thirty minutes was timed from the moment the temperature of the milk in the control vials and the temperature of the water bath had reached the desired point.
Young (sixteen to twenty-hour) cultures of streptococci in dextrose-brain broth, on isolation and after prolonged cultivation on artificial mediums, were used to inoculate the autoclaved milk to be heated. Approximately 0.02 c.c. of the dextrose-brain broth culture, or about 1,000,000 organisms, was inoculated per cubic centimeter of the autoclaved milk. To simulate commercial conditions in the handling and use of milk, samples from supplies to be tested and the inoculated specimens often were placed in the refrigerator at 10° C. overnight or longer and then kept at room temperature for short periods before heating. Samples of raw and pasteurized milk and the suspensions of streptococci in autoclaved milk were heated for thirty minutes at 63° C. (145.4° F.), 68° C. (154.4° F.) and 73° C. (163.4 ° F.), respectively. To determine the presence of viable organisms after heating, subcultures were made routinely in dextrose-brain broth, and often also in dextrose broth, autoclaved milk and on blood-agar, before and after heating.
Rabbits were inoculated intravenously with 0.5 c.c. of undiluted dextrose-brain broth culture per 100 gm. of body weight, and intracerebrally with 0.1 c.c. of 1:200 to 1:10,000 dilutions of eighteen-hour dextrose-brain broth cultures of the streptococci under study. Mice were inoculated intracerebrally with 0.03 c.c. of 1:200 to 1:10,000 dilutions, intraperitoneally with 1.2 c.c. and intranasally, while under deep ether anesthesia, with 0.05 c.c. of the undiluted eighteen-hour dextrose-brain broth cultures of the streptococci.
The distribution curves of cataphoretic velocity and the incidence of agglutination of the streptococci by the respective antistreptococcic serums of comparable strength were determined by methods previously described.13,17
Results of Cultures
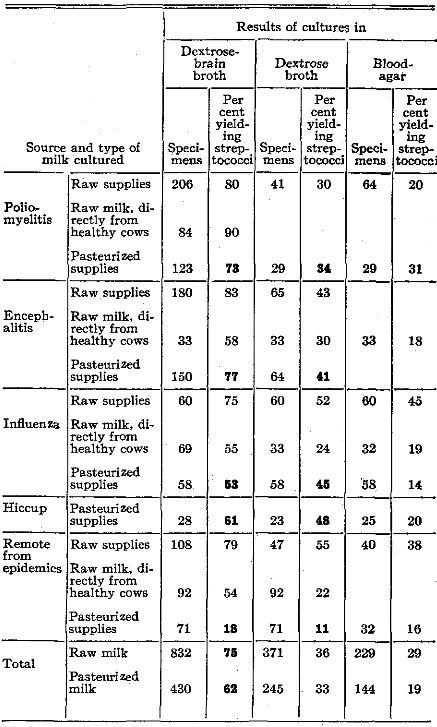
The incidence of isolations of streptococci in dextrose-brain broth, in dextrose broth and on blood-agar from raw and pasteurized milk supplies and from raw milk obtained in a sterile manner directly from cows, in relation to epidemic diseases and interepidemic periods, is summarized in Table I. It will be seen that the incidence of isolations of streptococci from the three types of milk cultured, but especially from composite raw milk, was uniformly higher, and in most instances much higher, in dextrose-brain broth than in dextrose broth and on blood-agar. There was a much higher incidence of isolation of streptococci from pasteurized samples during epidemic periods than from pasteurized samples during periods remote from epidemics, ranging from 77 per cent during to 18 per cent remote from epidemics. Of 832 samples of raw milk, 75 per cent yielded streptococci in dextrose-brain broth; of 371 samples, 36 per cent yielded streptococci in dextrose broth and of 229 samples, streptococci grew on blood-agar in only 29 per cent. The average incidence of isolations of streptococci from commercially pasteurized milk was 62 per cent in dextrose-brain broth, 33 per cent in dextrose broth and 19 per cent on blood-agar.
Table I. Isolation of Alpha or Green-Producing Streptococci from Raw and Pasteurized Milk Supplies in Relation to Epidemic Diseases
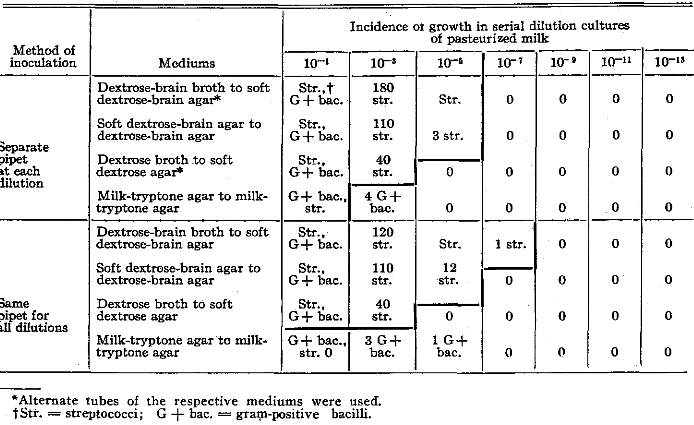
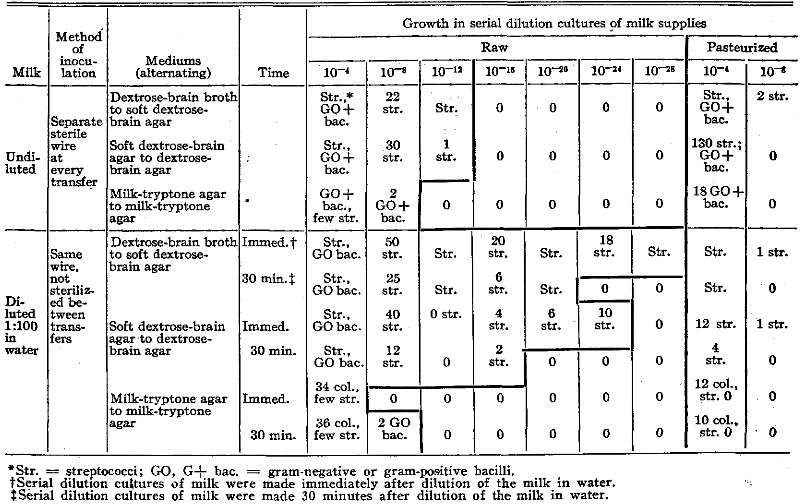
The comparative results from the use of different culture mediums in serial dilution cultures for the isolation of streptococci from raw and pasteurized milk are well illustrated in Tables Il, III and IV. The samples cultured were from a milk supply during a mild epidemic of infection of the upper respiratory tract. The sample of pasteurized milk cultured, in serial dilutions at steps of 10-2, the results of which are shown in Table II, was obtained in the open market and cultures were made immediately. Colony counts, by plating 1 c.c. of a 1:100 (10-2) dilution in milk-tryptone agar, revealed four colonies of bacilli or 400 colonies per cubic centimeter of milk and no colonies of streptococci, whereas streptococci grew in dextrose-brain broth and dextrose-brain agar at dilutions up to and including 10-5 using separate pipets, and up to 10-7 using the same pipet in making the transfers. The samples of raw and pasteurized milk, cultured in serial dilutions at steps of 10-4, the results of which are shown in Table III, represent a pool of twelve samples of raw milk and the same twelve samples after pasteurization in the laboratory. It will be noted that growth of streptococci occurred in cultures of both the raw and pasteurized milk in the brain-containing mediums more often and in higher dilutions and in larger numbers than in corresponding dilutions in the standard medium, milk-tryptone agar, used routinely for determining the bacterial content of dairy products.1
Table II. Comparative Results from the Use of Different Mediums for the Isolation of Alpha Streptococci in Serial Dilution Cultures of Pasteurized Milk
Table III. Comparative Results from the Use of Different Mediums for the Isolation of Alpha Streptococci in Serial Dilution Cultures of Corresponding Samples of Raw & Pasteurized Milk
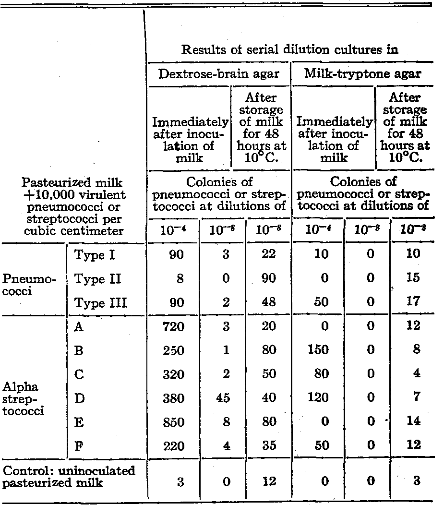
Table IV. Growth of Virulent Pneumococci and Alpha Streptococci in Pasteurized Milk at 10°C.
In instances in which milk supplies appeared to be responsible for the occurrence of outbreaks of disease, as referred to later, the milk had been stored for some time or was inadequately refrigerated. Hence, studies were made with my methods to determine whether virulent pneumococci or streptococci added to milk and whether streptococci or other organisms already present in the milk might multiply when kept at standard refrigerator temperatures. Results of these studies are well illustrated in Table IV. Separate, previously sterilized wires were used in making serial dilution cultures in soft dextrose-brain agar and milk-tryptone agar. The sample of pasteurized milk was obtained on the open market during a mild outbreak of infections of the respiratory tract. Twenty cubic centimeter amounts of pasteurized milk were placed in a series of test tubes and approximately 10,000 virulent pneumococci or streptococci were added per cubic centimeter. Dilution cultures at 10-4 and 10-8 were made immediately and again after storage at 10° C. for forty-eight hours. Estimates of the number of colonies of pneumococci or streptococci that grew in dextrose-brain agar and in the milk-agar plates were made after the respective cultures had been incubated for forty-eight hours. It was found (1) that the number of colonies of pneumococci or streptococci that grew at dilutions of both 10-4 and 10-5 in the test cultures made immediately and after refrigeration at 10° C. for forty-eight hours was far greater in soft dextrose-brain agar than in milk-tryptone agar; (2) that the number of colonies of pneumococci or streptococci that grew at 10-8 was far greater after the milk to which these organisms were added had been refrigerated for forty-eight hours than in cultures made immediately, and (3) that the streptococci which had resisted commercial pasteurization also grew at refrigerator temperature.
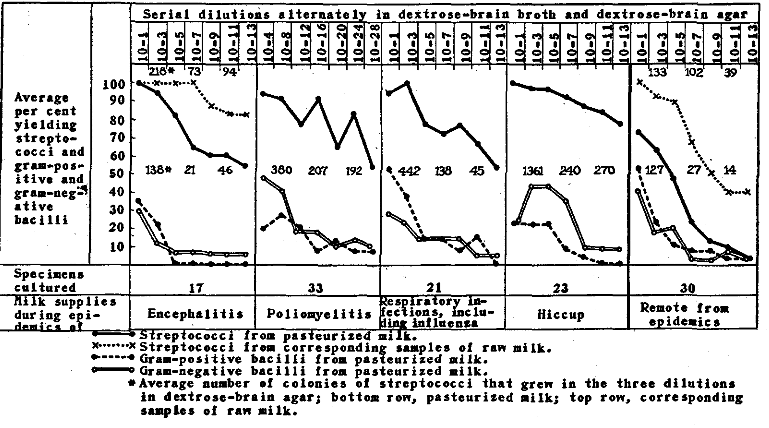
The incidence of growth of alpha streptococci and of gram-positive and gram-negative bacilli in serial dilution cultures, alternately in dextrose-brain broth and dextrose-brain agar, of milk supplies in relation to epidemics of encephalitis, poliomyelitis, infections of the respiratory tract including influenza, and hiccup and to periods remote from epidemics is shown graphically in Figure 1. Each dilution culture was made with the same sterile pipet or with the same wire sterilized only before and after the first transfer. It will be seen (1) that incidence of growth of streptococci was higher from raw than from pasteurized milk supplies during epidemics of encephalitis and remote from epidemics; (2) that the incidence of growth of streptococci from raw milk supplies cultured during epidemics of encephalitis, while about the same in low dilutions, was much greater in high dilutions than in corresponding cultures from raw milk supplies remote from epidemics; (3) that growth of streptococci from pasteurized milk supplies was consistently much higher, in both low and high dilutions, during epidemics of encephalitis, poliomyelitis, infections of the upper respiratory tract including influenza, and hiccup, than remote from epidemics; (4) that the incidence of growth of gram-positive and gram-negative bacilli from pasteurized milk supplies in the different dilutions, but especially in high dilutions, was far less than of streptococci and was about the same for epidemic and nonepidemic periods, and (5) that the average number of colonies of streptococci that grew in high dilutions in dextrose-brain agar was higher for raw than for pasteurized milk supplies, both during and remote from epidemics of encephalitis.
Fig.1. Growth of Alpha Streptococci and Gram-Positive and Gram-Negative Bacilli in Serial Dilution Cultures of Milk Supplies
The control colony counts, by the standard agar plate method, of samples of milk subjected to serial dilution cultures in the experiments summarized in Figure 1 and in many other experiments were usually well within prescribed limits. Streptococci almost never grew in the standard milk-agar plates at dilutions of more than 1:1,000 and never at dilutions greater than 10-8 in serial dilution cultures made in this medium, whereas corresponding dilution cultures made in the brain-containing mediums often yielded streptococci in far greater dilutions. Staphylococci were isolated infrequently from pasteurized milk. They were isolated more often from raw milk in low dilutions, but only occasionally in high dilutions.
The growth of streptococci in dilutions far greater than those believed possible on the basis of mathematical calculations of the original number of streptococci, considering streptococci as inert particles, is thought to be due to either “biogenesis” or growth of submicroscopic units while the dilutions are made or to differential adhesion of the streptococci, as such, or of submicroscopic components, to the wire or to the surface of the pipets used in making the dilutions. The dilutions, as indicated, represent dilution of fluids and not necessarily of organisms.
Virulence of the Streptococci
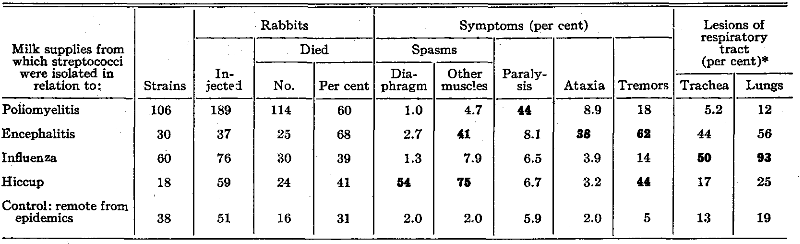
The results obtained after the intracerebral inoculation of rabbits with streptococci isolated from raw and pasteurized milk in relation to epidemics of poliomyelitis, encephalitis, influenza and hiccup, and remote from epidemics, are summarized in Table V. It will be seen that the respective streptococci were highly specific.
Table V. Mortality Rate, Symptoms and Lesions After Intracerebral Inoculation of Rabbits with Streptococci Isolated from Milk Supplies in Relation to Epidemic Diseases
*Of animals that died.
From a study of streptococci as isolated from pasteurized milk by the serial dilution method, it was found that streptococci which grew at extremely high dilutions were usually specifically virulent. The following experiments will suffice to illustrate this point.
Young dextrose-brain broth cultures of fourteen strains of streptococci isolated in pure culture at dilutions ranging from 10-8 to 10-28 from pasteurized milk supplies during a major epidemic of poliomyelitis were inoculated intracerebrally into rabbits to determine specific virulence. Among twenty-one rabbits so inoculated, flaccid paralysis developed as the outstanding symptom in twelve, seven of which died. Moreover, when freshly isolated cultures of the streptococci were nebulized into the air of cages containing mice and added to the running water in which fish were kept, or when the streptococci were added to the drinking water of young mice, there occurred localization of the streptococci in the central nervous system, symptoms of encephalitis and formation of encephalitis virus,20 and death from encephalitis and flaccid paralysis,18,26 respectively, in significant incidence.
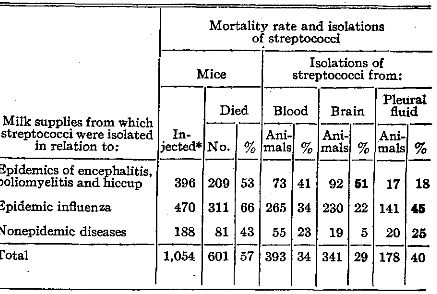
The results obtained in mice after intraperitoneal, intracerebral and intranasal inoculation of streptococci freshly isolated in dextrose-brain broth from raw and pasteurized milk are summarized in Table VI.
Table VI. Virulence for Mice of Streptococci Isolated from Milk Supplies in Relation to Epidemic Disease
*Intraperitoneally, intracerebrally or intranasally.
The mortality rate, invasion of the blood stream and the greater tendency of the streptococci isolated from milk during epidemic periods to localize electively in comparison to that of strains isolated from milk supplies remote from epidemics is strikingly shown.
Specificity of Streptococci as Shown by Cataphoresis
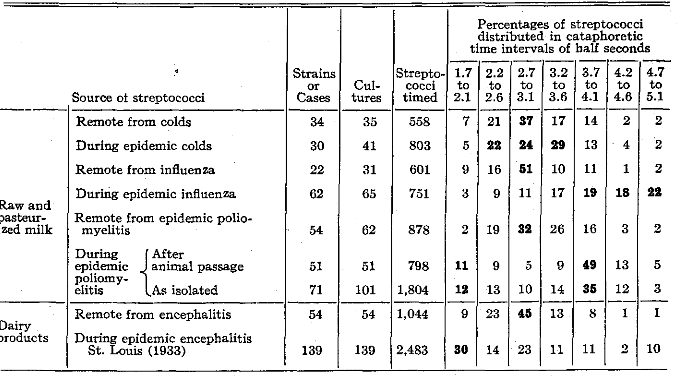
It has been shown elsewhere that alpha streptococci having virulence and other properties characteristic of streptococci associated with epidemic diseases occur commonly in milk and other dairy products, as well as in air, in water and in emulsions made of flies and mosquitoes at the time of epidemics.9,10,13 I have applied the cataphoretic method of study to strains of streptococci isolated from milk supplies.9,12,16 The distribution of cataphoretic time of streptococci isolated from raw and pasteurized milk and other dairy products during and remote from epidemics of colds, influenza, poliomyelitis and encephalitis is summarized in Table VII. The mode of the streptococci isolated from milk at the time of the respective epidemics was very different, and was characteristic of the streptococci isolated from patients suffering from the respective epidemic disease.13,27 In contrast, the mode of the streptococci isolated from milk remote from epidemics resembled that of streptococci isolated from the nasopharynges of well persons and persons who had diseases not caused by streptococci remote from epidemics, and of epidemic strains after prolonged cultivation on artificial mediums.
Table VII. Cataphoretic Time of Streptococci from Milk and Other Dairy Products in Relation to Epidemic Colds, Influenza, Poliomyelitis and Encephalitis and Interepidemic Periods
Serologic Specificity of Streptococci
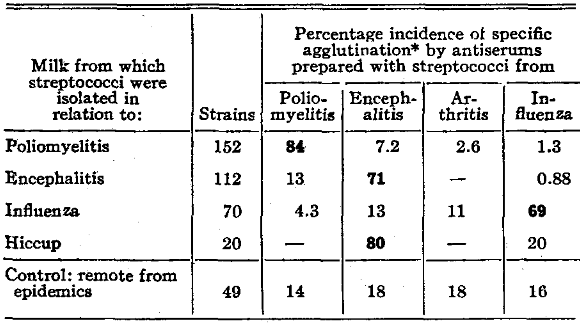
By the special methods used successfully in previous studies,17 a large number of agglutination experiments was carried out with the streptococci isolated from milk and other dairy products using convalescent human serum and the serum of horses hyperimmunized with streptococci obtained from persons who were ill with the respective diseases. The results obtained with the hyperimmune serums, according to epidemics, are summarized in Table VIII. A high degree of specificity was found for each of the groups of epidemic strains studied, which was not the case for strains isolated from milk remote from these epidemics. The specific agglutinin content of the serum of persons for the respective strains was found to be increased during convalescence.
Table VIII. Agglutination of Streptococci Isolated from Milk
*No specific agglutination by normal horse serum. Agglutination was considered specific if greater in the different dilutions of a given antiserum, or if it occurred in at least tenfold greater dilution of the specific antiserum, than of control antiserum.
Resistance to Heat of Epidemic and Nonepidemic Strains of Alpha Streptococci
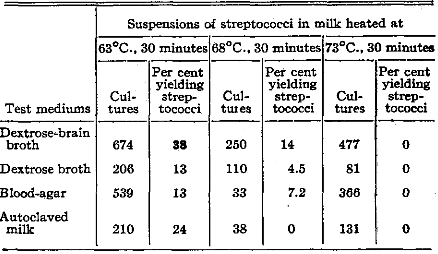
Streptococci from various sources, on isolation and after prolonged cultivation on artificial mediums, were suspended in autoclaved milk and heated at 63, 68 and 73° C. (145.4, 154.4 and 163.4° F.) for thirty minutes to test resistance of the various strains to heat. Cultures were then made routinely in dextrose-brain broth, and frequently also in dextrose broth, in autoclaved milk and on blood-agar plates. The importance of the use of a highly favorable medium, such as dextrose-brain broth, to determine whether the streptococci resisted heating at the different temperatures, is shown in Table IX. After heating at 63°C. (145.4° F.) (pasteurizing temperature), the incidence of isolation of streptococci in dextrose-brain broth was uniformly higher (38 per cent) than in autoclaved milk (24 per cent), dextrose broth (13 per cent) and blood-agar (13 per cent). Heating at 68° C. (154.4° F.) for thirty minutes, and at 73° C. (163.4° F.) for ten or twenty minutes did not suffice to kill all streptococci in milk, whereas heating at 73°C. (163.4° F.) for thirty minutes invariably did suffice. On the basis of these results, dextrose-brain broth was used routinely for making cultures from milk supplies as obtained at the time of study, after pasteurization of raw milk and after repasteurization, under controlled condition in the laboratory, of commercially pasteurized milk, and for testing the heat-resistance of streptococci suspended in milk.
Table IX. Comparative Value of Different Culture Mediums in Determining the Thermal Death Point of Streptococci Suspended in Autoclaved Milk
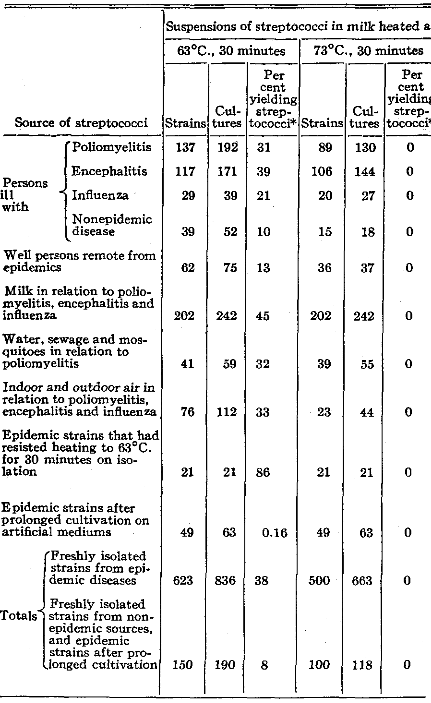
The total incidence of isolations of streptococci in dextrose-brain broth after pasteurization or heating (63° C. [145.4° F.] and 73° C. [ 163.4° F.] for thirty minutes under controlled conditions) of suspensions of streptococci in milk is summarized in Table X. The incidence of isolation of streptococci after pasteurization at the usual temperature was highest (86 per cent) in the case of epidemic strains that had resisted previous commercial or laboratory pasteurization and was next highest in the case of epidemic strains obtained from milk supplies (4S per cent), and from persons having epidemic encephalitis (39 per cent). The incidence of isolation after pasteurization in milk of streptococci obtained from persons having poliomyelitis (31 per cent) or influenza (21 per cent), from indoor and outdoor air (33 per cent) and from water (32 per cent) in relation to poliomyelitis, encephalitis and influenza, also was significantly higher than after pasteurization of streptococci obtained from well persons (13 per cent) or persons ill with chronic disease (10 per cent) remote from epidemics and than after pasteurization of epidemic strains after prolonged cultivation on artificial mediums (0.16 per cent). Thirty-eight per cent of 836 cultures of streptococci representing 623 epidemic strains, and 8 per cent of 190 cultures representing 150 nonepidemic strains, resisted pasteurization at 63° C. (145.4° F.) for thirty minutes. Pasteurization at 73° C. (163.4° F.) for thirty minutes sufficed to kill the streptococci in every instance, regardless of their source or time after isolation.
Table X. Resistance to Heat of Alpha Streptococci on Isolation and After Prolonged Cultivation in Relation to Epidemic and Nonepidemic Diseases
*In dextrose-brain broth cultures.
To check further the technical procedures used in these studies, autoclaved milk was inoculated with mixtures of young cultures of Bacillus subtilis, Escherichia coli, hemolytic or beta type of streptococci and staphylococci, and then pasteurized under controlled conditions at 63 ° C. (145.4° F.) for thirty minutes. Escherichia coli, beta type of streptococci and staphylococci were killed in every instance and Bacillus subtilis was killed in most instances.
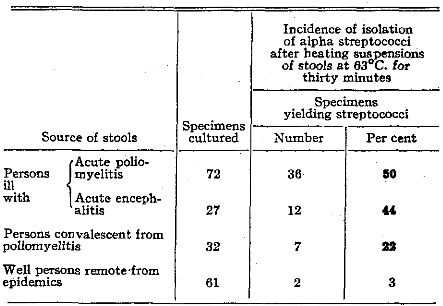
To compare the resistance to heat of streptococci that had grown in vivo with that of the freshly isolated alpha streptococci associated with epidemic and other diseases and those from well persons remote from epidemics, 10 per cent emulsions in saline solution of stools of patients who had poliomyelitis or encephalitis and emulsions of stools of well persons remote from epidemics were diluted threefold in saline solution and heated at 63° C. (145.4° F.) for thirty minutes in the laboratory under controlled conditions. Sterility tests were made in dextrose-brain broth. The scope and results of these experiments are shown in Table XI. Alpha streptococci, nearly always in mixture with gram-positive bacilli (Clostridium perfringens) and only occasionally with Escherichia coli, were isolated far more often from pasteurized suspensions of stool specimens that had been obtained from persons ill with poliomyelitis (50 per cent) or encephalitis (44 per cent) than from persons convalescent from poliomyelitis (22 per cent) and than from well persons remote from epidemics (3 per cent).
Table XI. Incidence of Isolation of Alpha Streptococci from Stools After Heating at 63°C. for Thirty Minutes
Epidemiologic Significance of Streptococci Isolated from Milk
Evidence was not lacking that milk supplies from which specific types of alpha streptococci were isolated were responsible for epidemic outbreaks and sporadic cases. One institutional outbreak of acute poliomyelitis at a college was traced to milk.10 Spread of the disease stopped abruptly when the use of the milk in which large numbers of the poliomyelitic type of streptococcus were demonstrated was discontinued.
A rural outbreak of poliomyelitis27 was traced to improperly refrigerated raw milk that was supplied by several dairies, in the herds of which the streptococcus was demonstrated in milk obtained directly from cows. In a major outbreak of poliomyelitis,28 streptococci having “poliomyelitic” cataphoretic velocity and which produced flaccid paralysis in rabbits were isolated from a brand of pasteurized milk supplied to families in which the incidence of poliomyelitis was far greater than in families in which other brands of pasteurized milk were used and from which this type of streptococcus was not obtained. In still another epidemic of poliomyelitis14 in which several brands of milk were used, milk obtained where cases had occurred revealed the streptococcus whereas no cases could be traced to the milk from which the streptococcus could not be isolated and which, through the foresight of the dairyman, was pasteurized at 155° F. instead of at the usual 145° F. In many instances composite milk supplies and milk obtained in a sterile manner directly from cows (which usually showed no evidence of disease of udders) supplying the milk for isolated family groups where one or more cases of poliomyelitis, encephalitis,22 influenza or persistent hiccup had occurred were shown to contain the respective specific types of streptococci. In one institutional outbreak of influenza the alpha type of streptococcic flora obtained from the nasopharynges of patients and similar flora contained in suspensions of a brand of cheese which the patients had consumed were indistinguishable. The epidemic disappeared promptly after the cheese was eliminated from the diet.
During institutional and community outbreaks of influenza, the number of colonies of streptococci that grew in soft dextrose-brain agar and on blood-agar and the pneumotropic virulence of the streptococci, as demonstrated by inoculation of animals with streptococci isolated in dextrose-brain broth from raw and pasteurized milk, were uniformly much higher than in the case of the same milk supplies three months after the epidemic had disappeared.
An institutional outbreak of acute appendicitis was traced to ice cream and an outbreak of epidemic parotitis (mumps) was traced to butter and cheese from which alpha streptococci that produced appendicitis in rabbits and parotitis in dogs were isolated.23 The ice cream was a local product, but the butter and cheese had been manufactured far remote from the outbreak studied, at a time when epidemic parotitis was prevalent. An epidemic of sore throat associated with a high incidence of myositis was traced to a streptococcus in the milk supply.24 The streptococcus, on isolation from throats of patients and from the milk, produced myositis in rabbits following intravenous injection.
Milk supplies, even pasteurized supplies, sometimes appeared to be responsible for the persistence of mild symptoms after attacks of epidemic disease, and for mild nonepidemic conditions in which the milk supplies were not considered as a possible source of infection. In several cases of perforating gastric ulcer and of gastric hemorrhage due to ulcer, the milk used was found to contain large numbers of the ulcer-producing type of streptococcus. Slight fever among patients convalescing from epidemic poliomyelitis and encephalitis and symptoms, such as persistent cough and recurring sore throat, after attacks of colds and influenza often disappeared when the respective milk supplies from which the streptococci were isolated were boiled or were eliminated.
Discussion and Summary
Results of these studies on alpha streptococci in relation to milk supplies are in accord with results of other workers, but through the use of brain-containing mediums they have been carried a step further, in that the incidence of isolation of streptococci has been higher and in that specificity of streptococci characteristic of those associated with certain epidemic and nonepidemic diseases has been demonstrated. The brain-containing mediums, especially in serial dilution cultures, were essential for the isolation of the virulent, epidemic strains without loss of specificity. The isolation of alpha streptococci from milk after pasteurization has been reported by Ayers and Johnson,2,3 Stark and Stark,33 Park,6 Bickwith and Eddie cited by Sears and Benson,29 Kitchen,4 Seibel30 and others. In the original experiments which led to pasteurization of milk as now practiced, only a few tests were performed on the resistance to heat of the alpha type of streptococci.5,6,7 These organisms isolated by methods then available were found more resistant to heat than hemolytic streptococci, but were considered as of little or no epidemiologic importance.7
The streptococci isolated by our methods from milk supplies during epidemics of encephalitis, poliomyelitis, influenza and hiccup manifested respective specific virulence or disease-producing properties and had characteristic distribution curves of cataphoretic velocity. They were agglutinated specifically by the respective antistreptococcic serums and they often grew in milk at usual refrigerator temperatures and in far higher serial dilutions in dextrose-brain broth and dextrose-brain agar than streptococci from milk supplies remote from epidemics, resembling, in these respects, the streptococci isolated from the respective patients and viruses.16 Streptococci present in milk during epidemics and those isolated from patients were unusually resistant to heat on isolation, often remaining viable, as shown by the use of dextrose-brain broth, after being subjected to commercial pasteurization and pasteurization under controlled conditions in the laboratory at 63° C. (145.4° F.) for thirty minutes. The specific properties, including high resistance to heat, disappeared abruptly on cultivation on the usual mediums and more slowly on cultivation in the brain-containing mediums. The relation of the streptococci isolated in these studies to Streptococcus durans or Streptococcus zymogenes isolated from pasteurized milk by Sherman and Wing31 was not determined.
Clinical and experimental evidence obtained indicates (1) that raw, and less often pasteurized, milk supplies shown to contain alpha streptococci true to type are probable sources of infection; (2) that during epidemics the streptococci normally present in respiratory and intestinal tracts of persons and broadly present in nature, including milk, acquire virulence and other properties characteristic of the streptococci associated with the respective epidemics; (3) that the incidence of diseases resulting from acquired specific virulence of the streptococci is increased by the drinking of milk containing the specifically virulent organisms.10
The experimental production from neurotropic or pneumotropic alpha streptococci of filtrable infectious agents resembling the viruses9,15,20,21 of encephalitis, poliomyelitis and influenza,25 respectively, and the demonstration of small, short chain forming diplococci in filtrates of poliomyelitis19 and encephalitis11 virus and in filtrates of experimental infectious agents produced from streptococci,19 indicate that epidemic types of streptococci in milk may be a source of the respective viruses. Regardless of whether specifically virulent alpha streptococci, which our methods have shown to be present consistently in raw and pasteurized milk supplies during epidemics, play a primary or secondary role in causation and spread of diseases now attributed to virus, the presence of viable streptococci in milk, even of those not at the moment virulent, should be regarded as an active or potential hazard to health and hence should be eliminated.
Pasteurization of milk by the holding and flash methods, as now practiced, while apparently adequate to kill beta streptococci, nonvirulent alpha streptococci and other pathogenic organisms commonly present in raw milk, has been found inadequate to kill specifically virulent alpha streptococci commonly present in milk supplies during epidemics of encephalitis, poliomyelitis, respiratory infections, influenza and hiccup. More efficient methods than are now generally used for the detection and killing of these organisms in milk are clearly indicated. To accomplish this ideal, slight, easily applicable modifications of methods now in general use fortunately have been found.
From the data obtained it is suggested (1) that in addition to the standard methods now in general use for the bacteriologic examination of milk and other dairy products without due regard to type or virulence of the organisms milk contains, dextrose-brain broth and dextrose-brain agar be used because highly favorable for the isolation of specifically virulent streptococci; (2) that growth of streptococci from raw and pasteurized milk supplies in high dilutions in these mediums be considered presumptive evidence of virulence of the organisms, and (3) that milk be pasteurized routinely at 73° C. (163.4° F.) for thirty minutes, or at least that it be pasteurized at this temperature during epidemics when, as has been shown, specifically virulent streptococci are present which resist the present-day holding and flash methods of pasteurization. I am informed that pasteurization equipment now in general use could be adapted to this higher temperature merely by adjustment of the temperature regulator. After pasteurization of bulk milk at this higher temperature the cream-line usually is not obliterated and the slight alteration of taste which occurs should not be considered objectionable, but rather as evidence that the milk was adequately heated to kill specifically virulent as well as saprophytic alpha streptococci.
References Cited:
- American Public Health Association: Standard methods for the examination of dairy products; bacteriological, bioassay and chemical. Ed. 7. New York: American Public Health Association, 1939.
- Ayers, S. H., and Johnson, W. T., Jr.: Ability of streptococci to survive pasteurization. J. Agric. Research, 2:321-330, 1914.
- Ayers, S. H., and Johnson, W. T., Jr.: Studies on pasteurization. XI. The “majority” and “absolute” thermal death points of bacteria in relation to pasteurization. XII. Cause and significance of pinpoint colonies from pasteurized milk. J. Bact., 9:279-300, (May) 1924.
- Kitchen, J. M. W.: Milk bacteria which proliferate before, and those which survive pasteurization: new methods applied to meet an as yet unremoved menace. M. Rec., 92: 409-414, (Sept. 8) 1917.
- North, C. E., Park, W. H., Moore, V. A., Rosenau, M. J., Armstrong, Charles., Wadsworth, A. B., and Phelps, E. B.: Commercial pasteurization. U. S. Pub. Health Bull., No. 147, (Feb.) 1925.
- Park, W. H.: Thermal death point of streptococci. Am. J. Pub. Health, 18:710-714, (June) 1928.
- Rosenau, M. J.: The thermal death points of pathogenic microorganisms in milk. U. S. Hygienic Laboratory Bull., No. 42, (Jan.) 1908.
- Rosenow, E. C.: Elective localization of bacteria in the animal body. In Jordan, E. O., and Falk, I. S.: The newer knowledge of bacteriology and immunology. Chap. 43, pp. 576-589. Chicago: University of Chicago Press, 1928.
- Rosenow E. C.: The relation of streptococci to the filtrable virus of epizootic encephalitis of the fox. J. Infect. Dis., 48:304-334 (Mar.) 1931.
- Rosenow, E. C.: An institutional outbreak of poliomyelitis apparently due to a streptococcus in milk. J. Infect. Dis., 50:377-425, (May-June) 1932.
- Rosenow, E. C.: Observations with the Rife microscope of filter-passing forms of microorganisms. Science, 76: 192-193, (Aug. 26) 1932.
- Rosenow, E. C.: The relation of streptococci to the epidemic of encephalitis in St. Louis: preliminary report. Proc. Staff Meet., Mayo Clin., 8:559-563, (Sept. 13) 1933.
- Rosenow, E. C.: Cataphoretic velocity and virulence of streptococci isolated from throats of human beings, from raw milk, flies, water, sewage and air during epidemics of the common autumnal cold. Am. J. Hyg., 19:1-21, (Jan,) 1934.
- Rosenow, E. C.: Observations on the epidemic of acute anterior poliomyelitis in Havana, 1934. Proc. Staff Meet., Mayo Clin., 9:613-616, (Oct. JO) 1934.
- Rosenow E. C.: The relation of streptococci to the viruses of poliomyelitis and encephalitis: preliminary report. Proc. Staff Meet., Mayo Clin., 10:410-414, (June 26) 1935.
- Rosenow, E. C.: Isolation of bacteria from virus and phage by a serial dilution method. Arch. Path., 26:70-76, (July) 1938.
- Rosenow, E. C.: Recurring encephalomeningoradiculitis with fibromyositis following poliomyelitis: a bacteriologic study of sixty-four cases. Arch. Int. Med., 64:1197-1221, (Dec.) 1939.
- Rosenow, E. C.. Epidemic poliomyelitis, recurrent encephalomeningoradiculitis and fibromyositis in relation to streptococci obtained from a water supply. Arch. Int. Med., 67:531-545, (Mar.) 1941.
- Rosenow, E. C.: Microdiplococci in filtrates of natural and experimental poliomyelitis virus compared under the electron and light microscopes. Proc. Staff Meet., Mayo Clin., 17:99-106, (Feb. 18) 1942.
- Rosenow, E. C.: The relation of neurotropic streptococci to encephalitis and encephalitis virus. Proc. Staff Meet., Mayo Clin., 17:551-560, (Nov. 4) 1942.
- Rosenow, E. C.: Studies on the relation of a neurotropic streptococcus and virus to epizootic encephalitis of wild ducks. Cornell Vet., 33:277-304, (July) 1943.
- Rosenow, E. C., and Caldwell, H. W.: Studies on the etiology and serum treatment of encephalitis during the epidemic in North Dakota and Minnesota (1941). Proc. Staff Meet., Mayo Clin., 16:587-588, (Sept. 10) 1941; Ann. Int. Med., 17:474-485, (Sept.) 1942.
- Rosenow, E. C. and Dunlap, Stella I.: An epidemic of appendicitis and parotitis probably due to streptococci contained in dairy products. J. Infect. Dis., 18:383-390, (Apr.) 1916.
- Rosenow, E. C., and Monn, V. H.: On an epidemic of sore throat and the virulence of streptococci isolated from the milk. J. Infect. Dis., 17:699-671, (July) 1915.
- Rosenow, E. C., and Williams, H. L.: Unpublished data.
- Rosenow, E. C., Heilman, F. R., and Pettet, C. H.: Observations on the epidemic of polio-encephalitis in Los Angeles, 1934. Proc. Staff Meet., Mayo Clin., 9:443-451, (July 25) 1934.
- Rosenow, E. C., Rozendaal, H. M., and Thorsness, E. T.: Acute poliomyelitis; studies of streptococci isolated from throats and raw milk in relation to one epidemic. J. Pediat., 2:568-593, (May) 1933.
- Rosenow, E. C., South, Lillian, H., and McCormack, A. T.: Bacteriologic and serologic studies in the epidemic of poliomyelitis in Kentucky, 1935. Kentucky M. J., 35: 437-446, (Sept.) 1937.
- Sears, H. J., and Benson, R. L.: Pathogenic streptococci and milk pasteurization. Am. J. Pub. Health, 13:937-940, (Nov.) 1923.
- Seibel, E. E.: Hitzefeste Bakterien in der bei 63° C. ½ Stunde Dauer pasteurisierten Milch. pp. 41-79. Berlin: J. Springer, 1926.
- Sherman J. M., and Wing, Helen U.: Streptococcus durans or Streptococcus Zymogenes isolated from pasteurized milk. J. Dairy Sc., 20:3-15, 1937.
- Soper, H. W.: Milk. Arch. Pediat., 60:1-9, (Jan.) 1943.
- Stark, C. N., and Stark, Pauline: The relative thermal death rates of young and mature bacterial cells. J. Bact., 18:333-337, (Nov.) 1929.