Access to all articles, new health classes, discounts in our store, and more!
Fertility, Prenatal & Childhood Nutrition
Stop Vitamin D Deficiency in Its Tracks: Raise Levels During Pregnancy

By Carole A. Baggerly
Vitamin D is one of the chemicals that our bodies use to regulate gene expression and produce compounds required for optimal cellular function. In fact, it is an essential hormone that affects over 3,000 cell processes. Without enough vitamin D circulating regularly in the blood, the body simply does not function as intended.
In its most extreme forms, vitamin D deficiency results in rickets in children and osteomalacia (bone softening) or osteoporosis (bone thinning) in adults. Milder degrees of deficiency or insufficiency have been associated with a vast array of chronic disorders, including impaired immune competence, autoimmune diseases (e.g., diabetes and multiple sclerosis), cancer (certain breast, colon, lung, and prostate cancers and lymphomas), high blood pressure, and cardiovascular disease, as well as pregnancy complications.
In order to determine whether your vitamin D status is deficient, insufficient, or sufficient, you need to take a 25-hydroxyvitamin D (25[OH]D) blood test. National Health and Nutrition Examination Survey (NHANES) data showed that approximately 99 percent of the U.S. population had 25(OH)D levels less than 50 ng/ml and the average level was around 25 ng/ml between 2001 and 2010.[1]
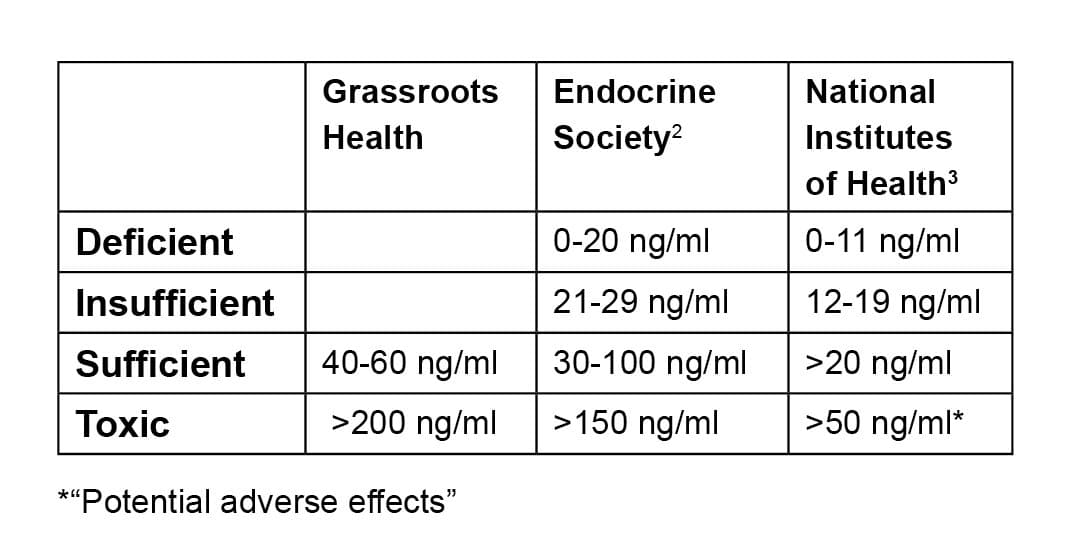
As seen in the table to the right, the National Institutes of Health states that vitamin D levels greater than 20 ng/ml are sufficient, and the Endocrine Society has determined sufficiency to start at 30 ng/ml. However, GrassrootsHealth, a nonprofit public health research organization focused on raising global awareness about vitamin D, recommends a level of at least 40-60 ng/ml, based on the findings of a panel of 48 senior vitamin D researchers from around the world and our examination of the research to date. (The question of toxicity will be addressed later in this article.)
If the population of the United States were to increase their vitamin D levels to 40 ng/ml, we could expect to avert as many as 336,000 deaths each year.[4] This would include the prevention of an estimated 180,000 deaths from cardiovascular disease, 20,000 from colorectal cancer, 12,000 from breast cancer, 70,000 from other cancers, and 15,000 from Alzheimer’s disease. In addition to the reduction in deaths, direct costs of care for the associated diseases would be reduced by roughly $130 billion each year. Raising 25(OH)D concentrations appears to be the most efficient and cost-effective way to reduce the burden of disease and increase life expectancy in the US.
The public health river
In one version of “the upstream story,” a parable frequently cited in public health, a couple sitting by a river notice a distressed person floating by. They rescue the person but soon see more distressed people floating down the river. Curious as to why this is happening, they walk upriver and discover an unfenced ledge from which people have been falling. Instead of pulling people out of the river all day long, they decide to build a fence on the ledge to prevent the people from falling in. Problem solved!
We want to reduce the health impacts associated with vitamin D deficiency by avoiding the problem in the first place. Where better to start than with pregnant mothers-to-be? If we screen and supplement mothers, and get their vitamin D levels up to at least 40 ng/ml, the fetuses should get sufficient vitamin D to enable proper growth and development of their bones, brains, and immune systems. Vitamin D sufficiency helps reduce preterm birth and other complications of pregnancy, and it gives the child a better start to life.
Starting at the source of the problem – in utero
The NHANES data from 2005-2006 revealed that 93 percent of women aged 18-45 (childbearing age) had vitamin D levels below 40 ng/ml. For African American women, the figure was 100 percent, and it was 99 percent for Hispanic women.[1] Reaching and maintaining a vitamin D level of at least 40 ng/ml during pregnancy could drastically reduce the racial disparities found in common complications of pregnancy.
Two randomized controlled trials (RCTs) were done in South Carolina under the direction of Bruce Hollis, PhD, and Carol Wagner, MD, respectively. The first, published in June 2011, studied 350 pregnant women who were given vitamin D supplements in the amount of either 400 IU/day (the then-current daily recommended intake [DRI] for pregnant women), 2000 IU/day, or 4000 IU/day.[5] One of the key outcomes from this research was that 4000 IU/day was both safe and effective for preventing several comorbidities in pregnancy. This was groundbreaking at the time; in fact, the researchers had to get special permission to give participants 4000 IU/day, as it was more than the Food and Nutrition Board’s safe upper intake level of 2000 IU.
higher vitamin D levels in the pregnant mother led to better pregnancy outcomes and higher vitamin D levels in the baby at birth
The second, almost identical, RCT, published in 2013, involved 257 women in two South Carolina community centers.[6] This trial only included two randomized treatment groups – women given 2000 IU/day and those given 4000 IU/day. (The 400 IU/day group had been eliminated for ethical reasons because in the previous study, most women in this group did not achieve vitamin D sufficiency.) The findings were consistent with those of the earlier study in that higher vitamin D levels in the pregnant mother led to better pregnancy outcomes and higher vitamin D levels in the baby at birth.
The outcomes for both these studies were centered on supplement dosing groups. In a subsequent analysis, the data was reexamined with a focus on the resulting serum vitamin D level, regardless of dosing group.[7] This analysis found that women with a 25(OH)D level of at least 40 ng/ml had a 59 percent lower risk of preterm birth than those whose vitamin D level was less than or equal to 20 ng/ml.
Yet another analysis of the data from the two RCTs mentioned above showed a 44 percent reduction in hypertensive pregnancy disorders, a 26 percent reduction in bacterial vaginosis, and a 13 percent reduction in gestational diabetes in women with vitamin D levels greater than 32 ng/ml, as compared to those with levels below 32 ng/ml, within six weeks of giving birth.[8]
A separate cohort study at a hospital in Turkey tested 179 pregnant women for serum vitamin D levels mid-pregnancy and six months postpartum. The women were screened for postpartum depression one week, six weeks, and six months after giving birth. A 71 percent reduction in postpartum depression was found for those with serum levels of at least 20 ng/ml, as opposed to those with levels at or below 10 ng/ml.[9]
In November 2016, a study on the vitamin D status of pregnant women and the risk of preeclampsia was published. Mirzakhani et al. found that women who had vitamin D levels of at least 30 ng/ml in both early and late pregnancy – 10-18 weeks and 32-38 weeks of gestation, respectively – had a 72 percent lower risk of preeclampsia than those with vitamin D levels below 30 ng/ml in both time periods.[10] No cases of preeclampsia were diagnosed in women with vitamin D levels higher than 37 ng/ml in early pregnancy.
How does Vitamin A status affect babies?
A mother with sufficient vitamin D status – defined as at least 40 ng/ml – throughout her pregnancy produces healthier babies. Below are summaries of studies on respiratory function, learning and development, diabetes, and preeclampsia with respect to the vitamin D level of either the mother or the baby.
A Korean study found that babies with higher vitamin D levels (above 30 ng/ml) in their cord blood were less likely to have respiratory infections by six months of age than those born with levels below 10 ng/ml.[11] Specifically, researchers found a 70 percent lower prevalence of the common cold, 66 percent lower prevalence of ear infections, and 62 percent lower prevalence of lung inflammation. Noting that 90 percent of Korean newborns have vitamin D levels below 30 ng/ml, the authors asked for a change in public health practices to encourage women to supplement with vitamin D or spend more time outside during pregnancy.
An Australian study found that vitamin D levels below 18 ng/ml were significantly associated with language impairment.[12] This study enlisted 743 pregnant Caucasian women from Perth and tested their vitamin D levels at 18 weeks of gestation, dividing participants into quartiles based on vitamin D level. The researchers later analyzed the children’s behavior at 2, 5, 8, 10, 14, and 17 years of age and measured language development at 5 and 10 years of age. They found that children from mothers with vitamin D levels below 18 ng/ml were twice as likely to have language development problems than children born to mothers with vitamin D levels above 28 ng/ml, although no association between vitamin D and behavioral or emotional difficulties was seen.
Elina Hyppönen, PhD, and colleagues conducted a birth cohort study in Finland with an even longer-term approach to understanding the significance of childhood vitamin D levels.[13] The study, which ran from 1966 through 1997, investigated the hypothesis that vitamin D levels in early childhood would have a bearing on development of type 1 diabetes. The researchers enrolled 12,055 women – all the women who were due to deliver in 1966 in a certain region of Finland – and collected data during the infants’ first year of life. They recorded the frequency of vitamin D supplementation given to the infants as regular, irregular, or none and noted whether the dose was below, at, or above the recommended amount of 2000 IU/day. The primary outcome measure of the study was the diagnosis of type 1 diabetes by the end of 1997. The researchers found that babies who were given at least some vitamin D had an almost 80 percent lower risk of developing type 1 diabetes than those who were given none. Moreover, among the babies who regularly received vitamin D supplementation, those given at least the recommended dose of 2000 IU/day had an approximately 80 percent reduced risk, compared to those whose dosages were lower.
Hyppönen, working with another research team, later analyzed pregnancy outcomes of women who had been Finnish birth cohort participants in infancy, and found a 51 percent reduction in preeclampsia for those women who had received regular supplementation of vitamin D during their first year of life.[14] The researchers suggested in the study abstract that “vitamin D intake in infancy may affect long-term programming of the immune response pattern.”
RECOMMENDATIONS FOR MOTHERS-TO-BE AND NURSING MOTHERS
If you are pregnant, trying to become pregnant, or lactating, we recommend that you immediately start supplementing with 5000 IU/day and read the directions below for becoming vitamin D sufficient. If you know someone else who is pregnant, please share this information with her.
- The first step is to test your vitamin D level. There are many factors that affect vitamin D absorption, including body mass index, age, and health issues; thus, for a given dose, responses can vary sixfold. You can use an at-home test, such as the GrassrootsHealth screening kit (grassrootshealth.net/test), or you can obtain a test through your doctor. Whichever method you choose, make sure you get the numerical result – not just a “you are fine”- as practice does not always keep up with research and many labs and physicians will report 20 ng/ml as adequate.
- Read research to determine the vitamin D level you would like to reach. The GrassrootsHealth panel of scientists recommends 40-60 ng/ml for optimal health, but if you are experiencing a specific health condition, you might want to examine the research related to it. Every condition seems to have a particular level of serum vitamin D below which improvements occur as vitamin D level increases and above which improvements tend to stop or significantly slow down. For avoiding rickets, that level is 20 ng/ml, and for achieving healthy pregnancy outcomes, it is 40 ng/ml.
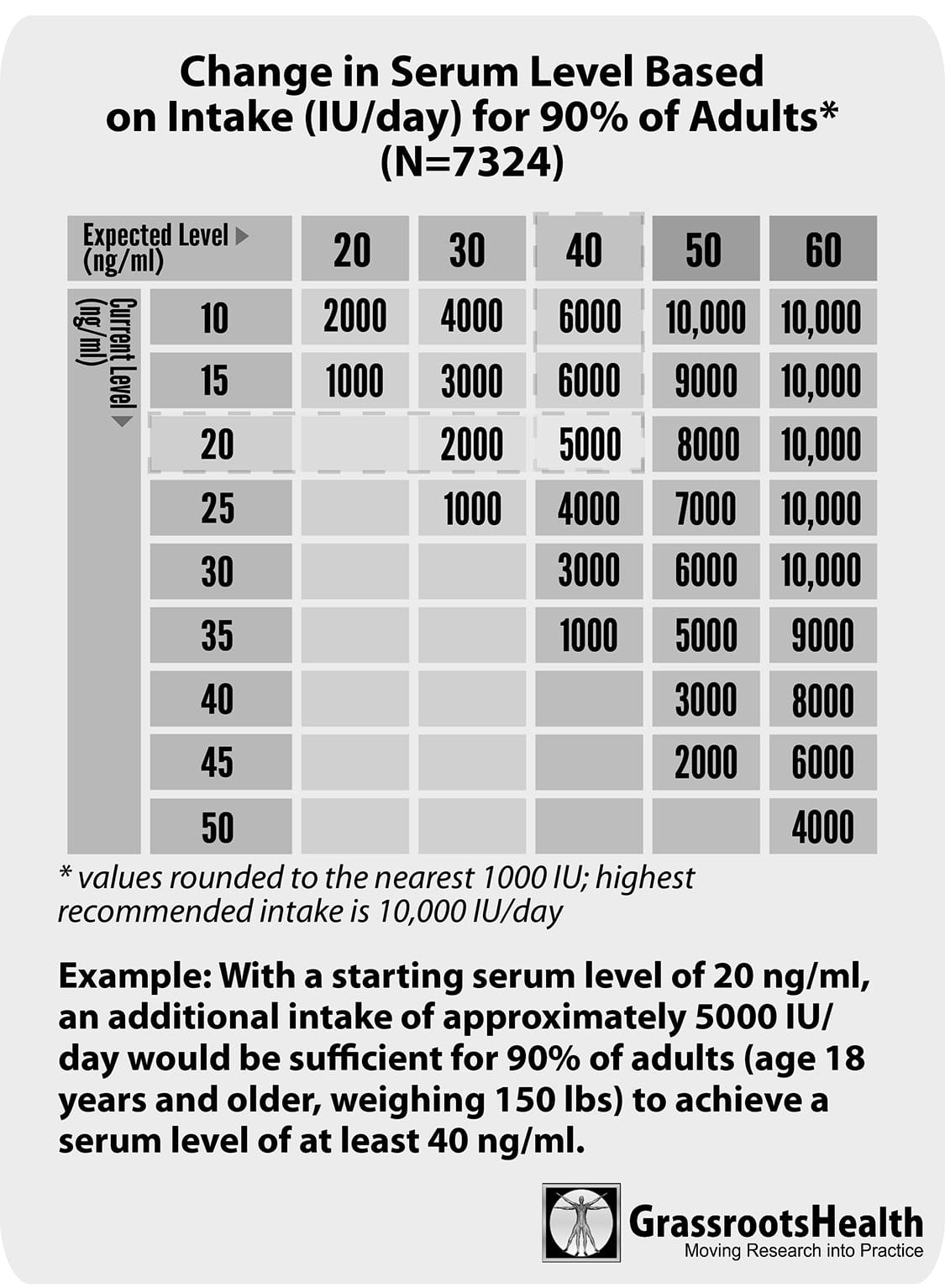
- Use the following chart to help guide you in changing your serum vitamin D level. This chart is based on data from over 7000 individuals in our participant self-study cohort. As part of our D*Action Project, participants screen their vitamin D levels from the comfort of their homes and provide us with information about their habits – such as supplement intake and sun exposure – and health conditions. (For more information, see grassrootshealth.net/index.php/daction.)
- Test again. It generally takes about two months for your vitamin D level to normalize after a change in practice (sun exposure, diet, or supplementation). After that time period, retest to see if you have reached your desired level. It may take several tries to find out what works for you and keeps you in your desired range.
Can sun exposure provide enough Vitamin D?
It is possible to get sufficient vitamin D from sunlight (or, when necessary, sun lamps), but it takes some effort to make sure you are getting enough, but not too much, daily exposure. Your skin type, your location, the season, and the time of day (Is it high noon in summer or 4 pm during the winter?) will help you determine how long you can stay in the sun without burning. Use the Vitamin D Council’s Sunshine Calendar (vitamindday.net/wp-content/uploads/2014/10/Sunshine-Calendar.pdf) to see if the sun is high enough in the sky to allow you to produce sufficient vitamin D. Also, ensure you are out during midday, between 11 am and 3 pm, or when your shadow is shorter than your height. Be careful not to get more than a “minimal erythema dose” of sun exposure; this is the amount of time it takes for you to be slightly pink the next day or to manufacture up to 20,000 IU of vitamin D. You can use apps such as dminder (dminder.ontometrics.com) to approximate this time until you are familiar with how your skin reacts to the sun. The important thing is to get regular, moderate UV exposure without burning.
Changing public health policy
Unfortunately, it can take an average of 17 years for research-based findings to be accepted in standard clinical practice. However, Grassroots- Health was founded on the premise of taking action and moving research into practice. Rather than waiting until 2034 for current findings to work their way through the conventional system, we have developed the Protect Our Children NOW! program to work with institutions that want to change their standard of care for pregnant women today. These institutions are helping their patients reap the benefits of healthier pregnancies, healthier babies, and reduced medical costs.
We provide the institution with a complete methodology for changing their standard of care, including guides and resources, engagement strategies, and education for staff and patients. We also gather patient data that can be used to help other institutions make the same changes, in the interest of affecting public policy.
With the new standard of care, driven by existing research, every woman has her vitamin D level measured upon her first obstetric visit, is given 5000 IU of vitamin D per day to start, and has follow-up tests at 24-28 weeks and 34-36 weeks of gestation. Throughout her pregnancy, doctors can modify the dosage as necessary to achieve vitamin D levels of at least 40 ng/ml. Vitamin D levels are recorded, and pregnancy outcomes are analyzed.
Staff members are expected to complete two free, online continuing medical education activities regarding vitamin D and pregnancy. (See grassrootshealth.net/vitamin-d-cmes.) They also receive weekly emails containing additional resources, charts, videos, and summaries of the latest research.
One key educational piece is informing the staff about the importance of testing versus blind supplementation. Providers are given the chart shown above to help them calculate the additional daily amount of vitamin D needed to get from a starting serum level to a target serum level. This chart is used in guiding pregnant women to achieve a level of at least 40 ng/ml after their initial vitamin D test.
Patients receive brochures and other print material, and they are given the opportunity to sign up for informative text messages and emails. All materials serve to educate them about the importance of vitamin D for themselves and their babies, as well as remind them to take their vitamin D supplement every day.
CASE STUDY: MEDICAL UNIVERSITY OF SOUTH CAROLINA
Our first Protect Our Children NOW! project was initiated at the Medical University of South Carolina (MUSC). Since September 2015, MUSC’s medical staff have seen over 3,000 pregnancies. Data collection is still underway, but we expect to have initial results analyzed and prepared for publication by mid-2017.
The first success at MUSC was obtaining buy-in from management. The director of women’s health research, Roger Newman, MD, has been supportive of this project from the beginning. His initial support came in part from the fact that the groundbreaking research of Hollis and Wagner had been conducted on site at MUSC. Despite this institutional connection, not everyone involved in the project was aware of vitamin D and its benefits. The project started with a free vitamin D test for all of MUSC’s obstetric staff. Out of 47 people tested, 41 had a vitamin D level below 40 ng/ml, which was certainly an eye-opening experience for them.
Another success of the project was receiving financial support from an insurance company, Select Health of South Carolina. With a potential outcome of decreasing preterm births by 50 percent – and given the fact that each preterm birth involves an added cost of $50,000 over a full-term birth – it was both a health- and cost-savings initiative for Select Health. At a rate of about 2000 births a year, 18 percent of which are preterm, it could save $9 million.
What about toxicity?
Vitamin D toxicity is a rare but potentially serious condition in which too high an intake of the vitamin causes abnormally high levels of calcium in the blood. If left untreated, it can lead to conditions such as high blood pressure, bone loss, and kidney damage. However, we have data showing that toxicity is virtually impossible with typical doses. It is worth noting that the standard of care at MUSC routinely involves the prescription of daily vitamin D supplementation over the tolerable upper limit – 4000 IU per day – set by the Institute of Medicine (IOM). Following is an excerpt from Newman’s vitamin D testing and treatment protocol, dealing with toxicity:
“Vitamin D toxicity is an uncertain entity and rarely encountered. Most labs will identify a 25(OH)D level of > 100-120 ng/ml as being potentially toxic. Toxicity is typically defined by elevations of the serum or urinary calcium levels and potentially kidney stones. We have not encountered any vitamin D levels that high either before or after supplementation. Nor have we encountered any side effects attributed to vitamin D supplementation. This experience includes several high dose vitamin D supplementation trials by Dr. Wagner. Published literature shows no toxicity under 200 ng/ml and 30,000 IU/day. This greatly exceeds any dosing regimen we would have.”
Is Vitamin D important to nursing mothers?
Yes! Lactating mothers should take 6400 IU of vitamin D daily (or receive the equivalent through sun exposure, if possible). This is based on research from Hollis and Wagner. In early 2000, they hypothesized that there was a safe amount of vitamin D that would give both mother and baby adequate nutritional vitamin D status. They compared 400 IU given to both the mother and the baby (the current DRI at the time for lactating mothers and infants) to 6400 IU given to the mother only (400 IU was from a standard prenatal vitamin and 6000 IU was added). Their first double-blind, randomized controlled study found that 6400 IU of vitamin D per day was safe, with no adverse reactions, and enabled mother and baby to achieve adequate nutritional vitamin D status.[15] This first study was small, with only 19 women, 15 of whom were Caucasian.
Encouraged by the results, they replicated the study with 258 women at two sites and a diverse population, which was about 25 percent African-American, 25 percent Hispanic, and 50 percent Causcasian.[16] This second study reported similar results. With 6400 IU of vitamin D daily, lactating mothers reached a mean vitamin D blood level of 60 ng/ml, and their babies reached a mean of 44 ng/ml (without direct supplementation). In the control group, mothers took only 400 IU of vitamin D per day and supplemented their children with 400 IU daily in the form of vitamin D drops. The mothers in this group achieved a mean of only 32 ng/ml (not nutritionally adequate), but the babies reached nutritionally adequate levels – a mean of 44 ng/ml – through supplementation. One of the most important take-away messages from this research is that breast milk can be an adequate source of vitamin D for the infant – if the mother takes enough of a supplement daily.
In earlier research, Hollis analyzed how vitamin D is transferred from the mother to the baby. He found that it is present in the breast milk primarily in its parent form as vitamin D3, rather than as 25(OH)D, the compound that is most commonly measured in blood. Although 25(OH)D has a half-life of approximately three weeks, vitamin D3 has a half-life of only about twelve hours and thus has to be replenished daily; intermittent dosing can maintain high levels in the blood but not in the breast milk.[17] For example, without daily dosing, breastfeeding mothers could have 50-60 ng/ml of 25(OH)D in their blood but no measurable vitamin D3 in their breast milk.
THE PROBLEM WITH CURRENT GOVERNMENT RECOMMENDATIONS
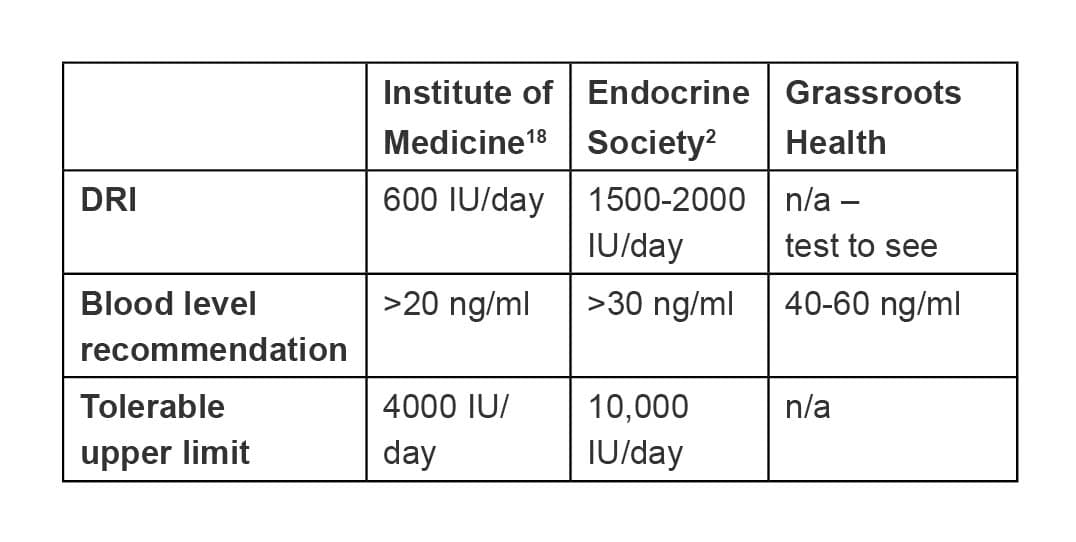
All of this research is enticing, but what usually stymies doctors and medical institutions from implementing these findings are government recommendations. They are far lower than any of the blood levels and daily dosages needed for optimal health.
GrassrootsHealth, along with numerous researchers, has three main concerns with the IOM’s vitamin D recommendations. The first is that the IOM based its recommendations on bone health alone. In its analysis, the institute concluded that there was not enough evidence to support any nonskeletal benefits of vitamin D. No evidence on benefits for cancer, cardiovascular health, autoimmune diseases, or pregnancy was considered.
Second, the IOM concluded that 20 ng/ml of 25(OH)D was sufficient to protect bone health. Research results, including data that was included in the IOM consideration, indicate that a minimum of 30 ng/ml is necessary for bone health. This was illustrated in a published response by Robert Heaney, MD, and Michael Holick, PhD, MD, to the IOM recommendation.[19] A minimum of 30 ng/ml for bone health was also determined by the Endocrine Society.
The third problem is a matter of statistics. The IOM came up with the current recommendations by analyzing studies and trying to get 97.5 percent of the population to a healthy level of bone function, specified as osteoid volume/bone volume less than 2 percent. They used data from a study that autopsied bone from 675 individuals who did not die of bone-related diseases.[20] The study examined the unmineralized osteoid and 25(OH)D levels to map bone health against vitamin D level. The IOM analysis of this study found only 7 individuals who failed to achieve the ideal level of bone mineralization at 20 ng/ml (7/675, or 1.03 percent), so they concluded that 20 ng/ml would get 99 percent of the population to a vitamin D level adequate for bone health.
Unfortunately, the IOM divided by the wrong number. They divided by the total number of individuals in the study (675), when they should have divided by 82, the number of individuals whose vitamin D levels were at or above 20 ng/ml. If they had divided by the correct number, they would have found that 7/82, or 8.5 percent, did not achieve a healthy level of bone mineralization at a vitamin D level of at least 20 ng/ml. Thus, their recommendation of 20 ng/ml only ensures that 91.5 percent of the population will have adequate vitamin D for bone health.
In contrast, GrassrootsHealth determined our recommended range of 40-60 ng/ml by examining a large number of studies that looked at vitamin D for both bone health and immune function. Our international panel of senior vitamin D researchers agrees that there should be a change to standard of care, to optimize vitamin D blood levels to 40-60 ng/ml. This will provide great improvements in public health, as well as helping pregnant and nursing mothers give their children the best possible start in life.
About the Author

ABOUT GRASSROOTSHEALTH
GrassrootsHealth is a nonprofit public health research organization dedicated to moving public health messages regarding vitamin D from research into practice. It is the recipient of the 2016 Humanitarian Award from the American College of Nutrition. GrassrootsHealth is currently running the D*action population intervention program to solve the vitamin D deficiency epidemic worldwide. Under the D*action umbrella, there are programs looking at the entire population, as well as targeted programs for breast cancer prevention and the Protect Our Children NOW! program. For more information, visit grassrootshealth.net.
REFERENCES
- Schleicher RL, Sternberg MR, Lacher DA, et al. The vitamin D status of the US population from 1988 to 2010 using standardized serum concentrations of 25-hydroxyvitamin D shows recent modest increases. Am J Clin Nutr. 2016; 104(2):454-461. doi: 10.3945/ajcn.115.127985.
- Holick MF, Binkley NC, Bischoff-Ferrari HA, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society Clinical Practice Guideline. J Clin Endocrinol Metab. 2011; 96(7):1911-1930. doi: 10.1210/jc.2011-0385.
- National Institutes of Health. Vitamin D: Fact Sheet for Health Professionals. https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/. Updated February 11, 2016.
- Grant WB. An estimate of the global reduction in mortality rates through doubling vitamin D levels. Eur J Clin Nutr. 2011; 65(9):1016-26. doi: 10.1038/ejcn.2011.68.
- Hollis BW, Johnson D, Hulsey TC, et al. Vitamin D supplementation during pregnancy: a double-blind, randomized clinical trial of safety and effectiveness. J Bone Min Res. 2011; 26(10);2341-2357. doi: 10.1002.jbmr.463.
- Wagner CL, McNeil R, Hamilton SA, et al. A randomized trial of vitamin D supplementation in 2 community health center networks in South Carolina. Am J Obstet Gynecol. 2013; 208(2):137.e1-13. doi: 10.1016/j.ajog.2012.10.888.
- Wagner CL, Baggerly C, McDonnell S, et al. Post-hoc analysis of vitamin D status and reduced risk of preterm birth in two vitamin D pregnancy cohorts compared with South Carolina March of Dimes 2009-2011 rates. J Steroid Biochem Mol Bio. 2016; 155:245-251. http://dx.doi.org/10.1016/j.jsbmb.2015.10.022.
- Wagner CL, McNeil RB, Johnson DD, et al. Health characteristics and outcomes of two randomized vitamin D supplementation trials during pregnancy: a combined analysis. J Steroid Biochem Mol Bio. 2013; 136:313-320. doi: 10.1016/j.jsbmb.2013.01.002.
- Gur EB et al. Mid-pregnancy vitamin D levels and postpartum depression. European Journal of Gynecology and Reproductive Biology. August 2014. http://www.ncbi.nlm.nih.gov/pubmed/24965990.
- Mirzakhani H, Litonjua AA, McElrath TF, et al. Early pregnancy vitamin D status and risk of preeclampsia. J Clin Invest. 2016; 126(12):4702-4715. doi:10.1172/JCI89031.
- Shin YH, Yu J, Kim KW, et al. Association between cord blood 25-hydroxyvitamin D concentrations and respiratory tract infections in the first 6 months of age in a Korean population: a birth cohort study (COCOA). Korean J Pediatr. 2013; 56(10):439-445. doi: 10.3345/kjp.2013.56.10.439.
- Whitehouse AJO, Holt BJ, Serralha M, et al. Maternal serum vitamin D levels during pregnancy and offspring neurocognitive development. Pediatrics. 2012; 129(3):485-493. doi:10.1542/peds.2011-2644.
- Hyppönen E, Läärä E, Reunanen A, et al. Intake of vitamin D and risk of type 1 diabetes: a birth-cohort study. Lancet. 2001; 358(9292):1500-1503. http://dx.doi.org/10.1016/S0140-6736(01)06580-1.
- Hyppönen E, Hartikainen A-L, Sovio U, et al. Does vitamin D supplementation in infancy reduce the risk of pre-eclampsia? Eur J Clin Nutr. 2007; 61:1136-1139. doi: 10.1038/sj.ejcn. 1602625.
- Wagner CL, Hulsey TC, Fanning D, et al. High-dose vitamin D3 supplementation in a cohort of breastfeeding mothers and their infants: a 6-month follow-up pilot study. Breastfeed Med. 2006; 1(2):59-70. doi: 10.1089/bfm.2006.1.59.
- Hollis BW, Wagner CL, Howard CR, et al. Maternal versus infant vitamin D supplementation during lactation: a randomized controlled trial. Pediatrics. 2015; 136(4):625-634. doi: 10.1542/peds.2015-1669.
- Hollis BW, Wagner CL. The role of the parent compound vitamin D with respect to metabolism and function: why clinical dose intervals can affect clinical outcomes. J Clin Endocrinol Metab. 2013; 98(12):4619-4628. doi: 10.1210/jc.2013-2653.
- Institute of Medicine Committee to Review Dietary Reference Intakes for Vitamin D and Calcium. Dietary Reference Intakes for Calcium and Vitamin D. Washington DC: National Academies Press; 2011. https://www.ncbi.nlm.nih.gov/books/NBK56070/.
- Heaney RP, Holick MF. Why the IOM recommendations for vitamin D are deficient. J Bone Miner Res. 2011; 26(3):455-457. doi: 10.1002/jbmr.328.
- Priemel M, von Domarus C, Klatte TO, et al. Bone mineralization defects and vitamin D deficiency: histomorphometric analysis of iliac crest bone biopsies and circulating 25-hydroxyvitamin D in 675 patients. J Bone Miner Res. 2010; 25(2):305-312. doi: 10.1359/jbmr.090728.
Published in the Price-Pottenger Journal of Health and Healing
Winter 2017 | Volume 40, Number 4
Copyright © 2017 Price-Pottenger Nutrition Foundation, Inc.®
All Rights Reserved Worldwide